For older people and frail people, the long-term benefit of medicines reduces and the potential for harm from adverse effects increases. When the benefit–risk balance changes in this way, medicine review and optimisation are important to simplify the therapeutic regimen, reduce inappropriate medicines and minimise risks. In this article, pharmacist prescriber Linda Bryant uses two case studies to illustrate important considerations during medicine reviews
Pterygium: A common presentation with cancerous masquerade conditions
Pterygium: A common presentation with cancerous masquerade conditions
We are on our summer break and the editorial office is closed until 17 January. In the meantime, please enjoy our Summer Hiatus series, an eclectic mix from our news and clinical archives and articles from The Conversation throughout the year. This article was first published in the 3 February edition
This article, by William Shew and Mo Ziaei, will help guide you through examination and treatment of pterygium, otherwise known as surfer’s eye
- Pterygia have a strong association with ultraviolet light exposure – the Coroneo effect results in nasal pterygium development.
- Topical lubricants are used for dry eye symptoms associated with pterygia, topical steroids may be used for inflamed pterygia, while surgery is reserved for severe cases.
- Sunglasses are important to prevent worsening or recurrence of pterygia.
This article has been endorsed by the RNZCGP and has been approved for up to 0.25 CME credits for continuing professional development purposes (1 credit per learning hour). To claim your credits, log in to your RNZCGP dashboard to record this activity in the CME component of your CPD programme.
Nurses may also find that reading this article and reflecting on their learning can count as a professional development activity with the Nursing Council of New Zealand (up to 0.25 PD hours).
Pterygium is a non-cancerous, triangular, fibrovascular membrane and one of the many ophthalmohelioses – ocular diseases where sunlight has been implicated in pathogenesis.
Pterygia are acquired conjunctival degenerations arising from repeated irritation of the ocular surface. Ultraviolet light exposure and other irritants, such as wind, dust and chronic infection, result in inactivation of tumour protein p53, cytokine release and growth factor release, leading to an arrest of apoptosis, inflammation and proliferation, respectively.1
This results in a localised nodule of accumulated degenerative elastin tissue known as a pinguecula. Once corneal migration of this fibrovascular tissue occurs, it is defined as a pterygium.
Pterygia may occur as early as age 20. Due to the strong association with UV exposure, risk factors include living in tropical climates, surfing and outdoor work.
New Zealand’s first ophthalmological survey in 1969 reported rates of pterygium in Māori to be 2.7 per cent,2 but more recent estimates are lacking. The Blue Mountains Eye Study in Australia reported a prevalence of 7.3 per cent.3
Human orbital anatomy is unique in that the lateral aspect of the eye is relatively exposed. Therefore, light entering from this aspect is focused onto a narrow area of the medial limbus, concentrating light up to 20 times (the Coroneo effect). This observation correlates with pterygia being located on the nasal aspect of the visible globe and in the dominant eye (the patient usually closes the non-dominant eye, which protects the globe).4
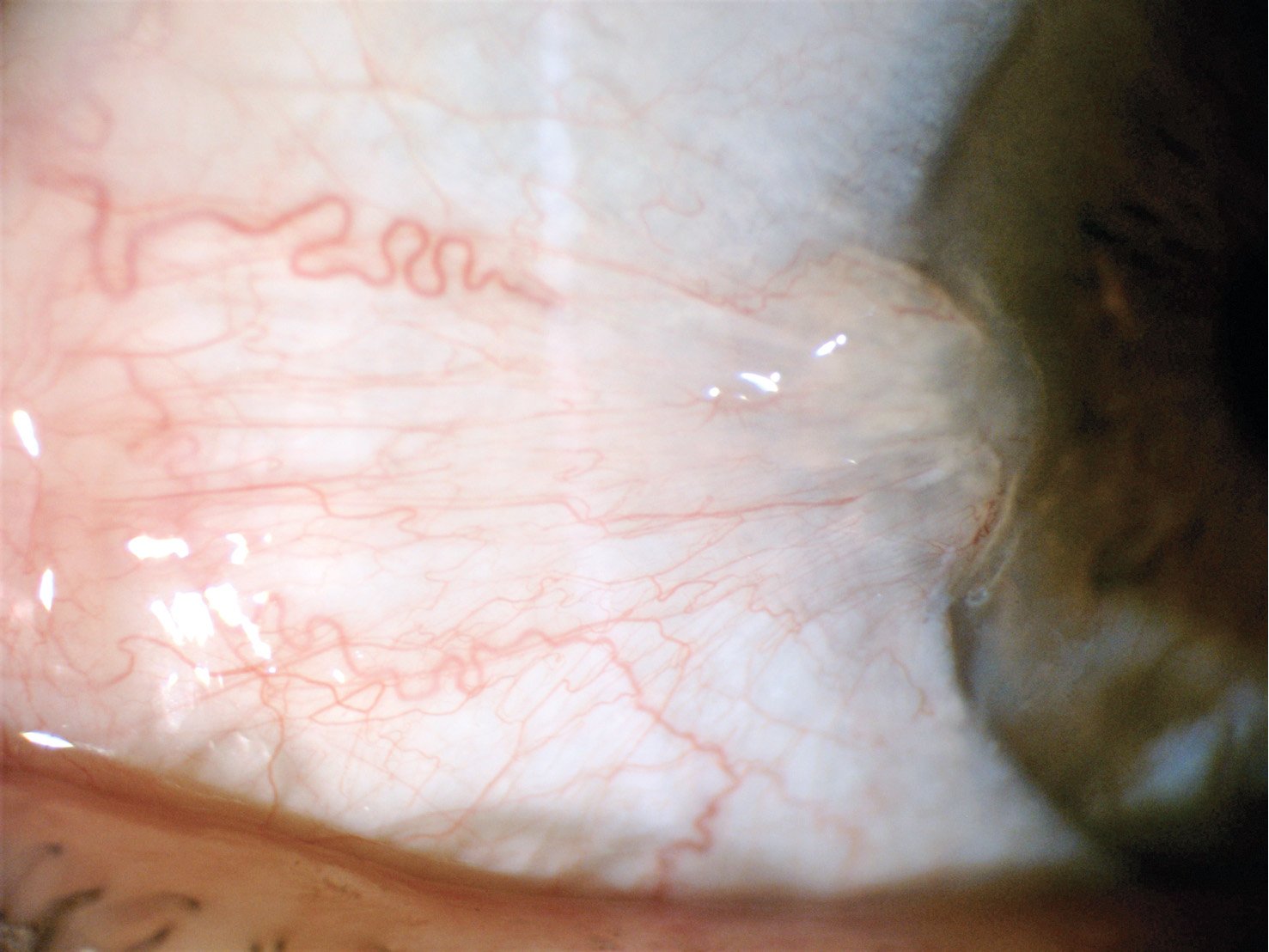
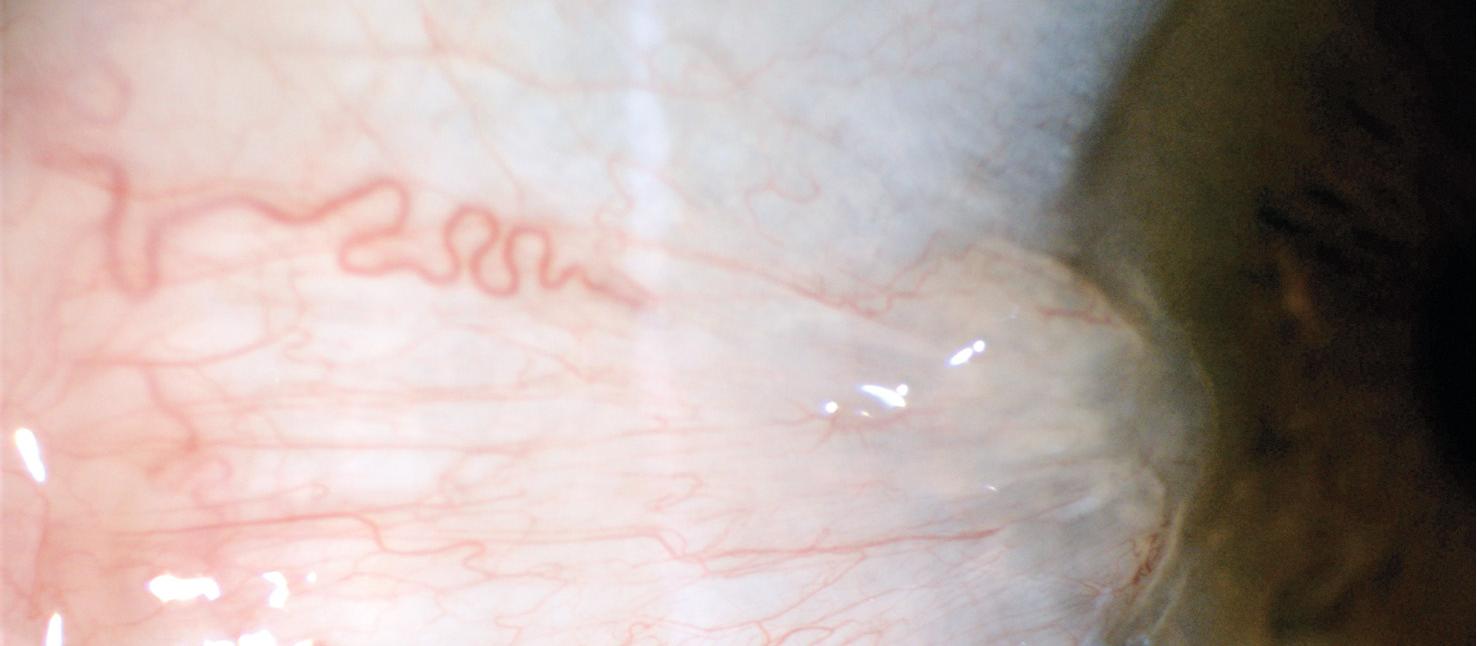
The typical lesion is a grey, vascularised, triangular membrane with the vessels and apex “dragged” towards the cornea (Figure 1). The membrane can vary in thickness from a thin, translucent appearance to a thick, fleshy growth. Ahead of the apex, under high magnification, a grey halo known as Fuchs patches can also be seen. Application of fluorescein may show staining over the pterygium itself or immediately around the edges of the pterygium, indicating dry areas due to poor spread of the ocular tear film.
Inflammation of the pterygium from dry eye and irritation can result in a symptomatic red eye with stinging, burning, foreign body sensation and frank pain. Patients may note that closure of the eyes (“resting” them) temporarily improves symptoms. Instillation of a short-acting topical anaesthetic will remove these symptoms, allowing the GP to confidently differentiate ocular surface pain from deeper inflammatory pain, such as scleritis or uveitis.
Growth of the pterygium may distort the cornea, inducing refractive error and resulting in blurring of unaided vision. Using a pinhole over the eye will usually result in a significant improvement in vision, allowing the GP to rule out visual loss from other causes.
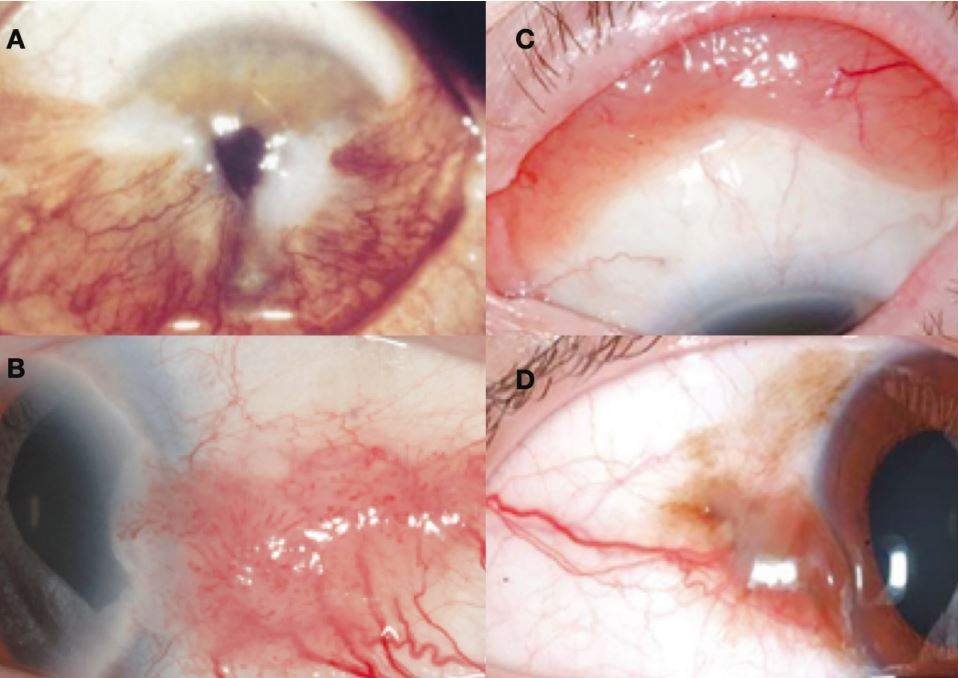
Patients with a pterygium should ideally be referred to a local optometrist for examination under slit lamp biomicroscopy and to be screened for masquerade conditions (several cancerous lesions can present as pterygium-like growth – common presentations are shown in Figure 2). However, if there are no suspicious features, patients can be simply observed as surgical treatment is not required in most cases.
Indications for referral include recurrent inflammation, induced refractive error, atypical location, rapid onset over weeks to months, immunosuppression and unusual vessel pattern.
A) Temporal and nasal pterygia – note that despite their severe appearance, they still respect the typical description of a dragged, triangular membrane in the visible portion of the eye (the lid has been retracted to show the protected upper globe).
B) Ocular surface squamous neoplasia – note the fleshy, gelatinous appearance with corkscrew vessels within the lesion. Additional feeder vessels supply the growth. These typically present in older patients, and risk factors include smoking and immunosuppression.
C) Conjunctival lymphoma – note the salmon-pink mass in the atypical location. Almost all are B-cell non-Hodgkin lymphoma cases, which typically occur in older adults and immunosuppressed individuals.
D) Conjunctival melanoma – note the feeder vessel overlying a pigmented, vascularised mass. These usually arise from long-standing pigmented lesions but can arise de novo, and there are variants that lack any pigmentation; therefore, assessment of the vessel pattern is vital. Typically occur in older adults.
All patients should wear well-fitted and wrapped sunglasses to prevent worsening of pterygia. While the AS/ NZS 1067.1:2016 standard is voluntary in New Zealand, most sunglasses sold here provide adequate protection against glare and UV. Patients should be advised to check labels and educated that UV light is not visible; therefore, the tint of the lenses has no correlation with UV-blocking ability.
Pterygia that produce significant dry eye symptoms should receive regular topical lubricants to cover areas that the natural ocular tear film neglects. A stepwise algorithm is used: initially, thin lubricant drops four times a day, increasing in frequency up to hourly, and changing to gel or ointment formulations for flare-ups.
Lubricants used more than four times a day should ideally be non-preserved; however, these are not funded and can be expensive if used for long periods. Overnight topical ointments to protect the eye from drying should be considered as some eyes may not fully close while sleeping.
Inflamed pterygia may require a short course of topical steroids as ongoing inflammation will further reinforce dry eye, thereby making lubricants ineffective. Corneal staining should be performed to rule out an epithelial defect before initiating therapy. Fluoromethalone 0.1 per cent is recommended as corneal esterases metabolise the steroids, preventing intraocular penetration. A typical regimen is two to four times a day for a maximum of one week.
Patients should be warned of long-term topical steroid side effects (raised intraocular pressure, cataract formation and eye infection due to local immunosuppression) to prevent them self-administering drops longer than intended. Lesions that do not settle after a week should prompt ophthalmology advice and/or referral if indicated.
Indications for surgical resection include corneal distortion, recurrent symptomatic flares and poor cosmesis. Younger patients seeking treatment may expect no less than a perfect outcome. Therefore, patients should be counselled that recurrence is possible, typically within the first year, and that recurrent pterygia can be larger than before.
Simple surgical excision has recurrence rates approaching 80 per cent; therefore, several adjunctive techniques are available to reduce recurrence. In New Zealand, the most common procedure involves harvesting a patch of conjunctiva from the superior aspect of the globe and placing this “autograft” onto the area of the excised pterygium.
While the autograft can be fixed using sutures, the most common way to achieve adherence is with tissue glue consisting of thrombin and fibrinogen, which provides patients with a significantly more comfortable recovery and a markedly reduced rate of recurrence (<5 per cent).
A video of pterygium excision using the conjunctival autograft and fibrin tissue glue technique can be found here: https://youtu.be/nhs9QYPhE30
Antimetabolites such a mitomycin C can also be used to further reduce the risk of recurrence, but their use is usually reserved for recurrent cases.
Pterygium excision is a day case procedure performed under local anaesthetic. It takes approximately 20 minutes and is very comfortable with the use of topical and subconjunctival anaesthesia, with or without sedation. Resected tissue is occasionally sent for biopsy to ensure a cancer is not missed.
Patients are advised to use regular mild analegisa for the first few days and are often able to return to work after 48 hours, especially if the lesion had been asymptomatic. A regimen of topical steroids for several weeks is used to reduce inflammation – a powerful stimulator of pterygium recurrence.
Patients may experience some ocular dryness, which can be allieviated with ocular drops as described earlier. Although many patients will only need one intervention, sunglasses should continue to be worn throughout their lives to prevent recurrence.
William Shew is a non-vocational registrar in ophthalmology in Auckland; Mo Ziaei is a cataract, cornea and anterior segment specialist at Greenlane Clinical Centre and Re:Vision Sight Correction Centre
You can use the Capture button below to record your time spent reading and your answers to the following learning reflection questions:
- Why did you choose this activity (how does it relate to your professional development plan learning goals)?
- What did you learn?
- How will you implement the new learning into your daily practice?
- Does this learning lead to any further activities that you could undertake (audit activities, peer discussions, etc)?
We're publishing this article as a FREE READ so it is FREE to read and EASY to share more widely. Please support us and our journalism – subscribe here
- Bradley JC, Yang W, Bradley RH, et al. The science of pterygia. Br J Ophthalmol 2010;94(7):815–20.
- Mann I, Potter D. Geographic ophthalmology: A preliminary study of the Maoris of New Zealand. Am J Ophthalmol 1969;67(3):358–69.
- Panchapakesan J, Hourihan F, Mitchell P. Prevalence of pterygium and pinguecula: the Blue Mountains Eye Study. Aust N Z J Ophthalmol 1998;26, Supp.1:2–5.
- Coroneo M. Ultraviolet radiation and the anterior eye. Eye Contact Lens 2011;37(4):214–24.