For older people and frail people, the long-term benefit of medicines reduces and the potential for harm from adverse effects increases. When the benefit–risk balance changes in this way, medicine review and optimisation are important to simplify the therapeutic regimen, reduce inappropriate medicines and minimise risks. In this article, pharmacist prescriber Linda Bryant uses two case studies to illustrate important considerations during medicine reviews
Switching blood pressure medications – it’s time to break the cilazapril habit
Switching blood pressure medications – it’s time to break the cilazapril habit
We're republishing this article in our Undoctored free access space so it can be read and shared more widely. Please think about supporting us and our journalism – subscribe here
HEARTBEAT
Last year, cilazapril with hydrochlorothiazide was discontinued, and now cilazapril alone is no longer funded for new patients. Consultant cardiologist Chris Ellis discusses what to do when patients with hypertension run out of their supply of these medications
- With recent changes to the funding of cilazapril, now is the time to switch patients to another medicine for treatment of hypertension.
- Angiotensin II receptor blockers offer equal efficacy to ACE inhibitors, but with fewer adverse effects.
- Candesartan 32mg plus chlorthalidone 12.5mg or indapamide 2.5mg is a stronger combination than losartan 50mg/ hydrochlorothiazide 12.5mg
This article has been endorsed by the RNZCGP and has been approved for up to 0.25 CME credits for the General Practice Educational Programme and continuing professional development purposes (1 credit per learning hour). To claim your credits, log in to your RNZCGP dashboard to record this activity in the CME component of your CPD programme.
Nurses may also find that reading this article and reflecting on their learning can count as a professional development activity with the Nursing Council of New Zealand (up to 0.25 PD hours).
A 69-year-old electrician with hypertension has been managed with medication for 19 years. He currently takes three tablets each morning and attends for a repeat prescription. He has heard that “his medicine” may no longer be available.
In 2002, he had been started on cilazapril at a dose of 0.5mg. This was gradually up-titrated to 5mg each morning. In 2010, he was changed to cilazapril 5mg with hydrochlorothiazide 12.5mg (Inhibace Plus). In 2015, amlodipine 2.5mg was added, along with atorvastatin 20mg daily to lower his overall cardiovascular risk.
He has also been encouraged to maintain the recognised lifestyle methods to lower his blood pressure: exercise more, lose weight, eat less salt, drink less alcohol and stop smoking (he has never smoked).
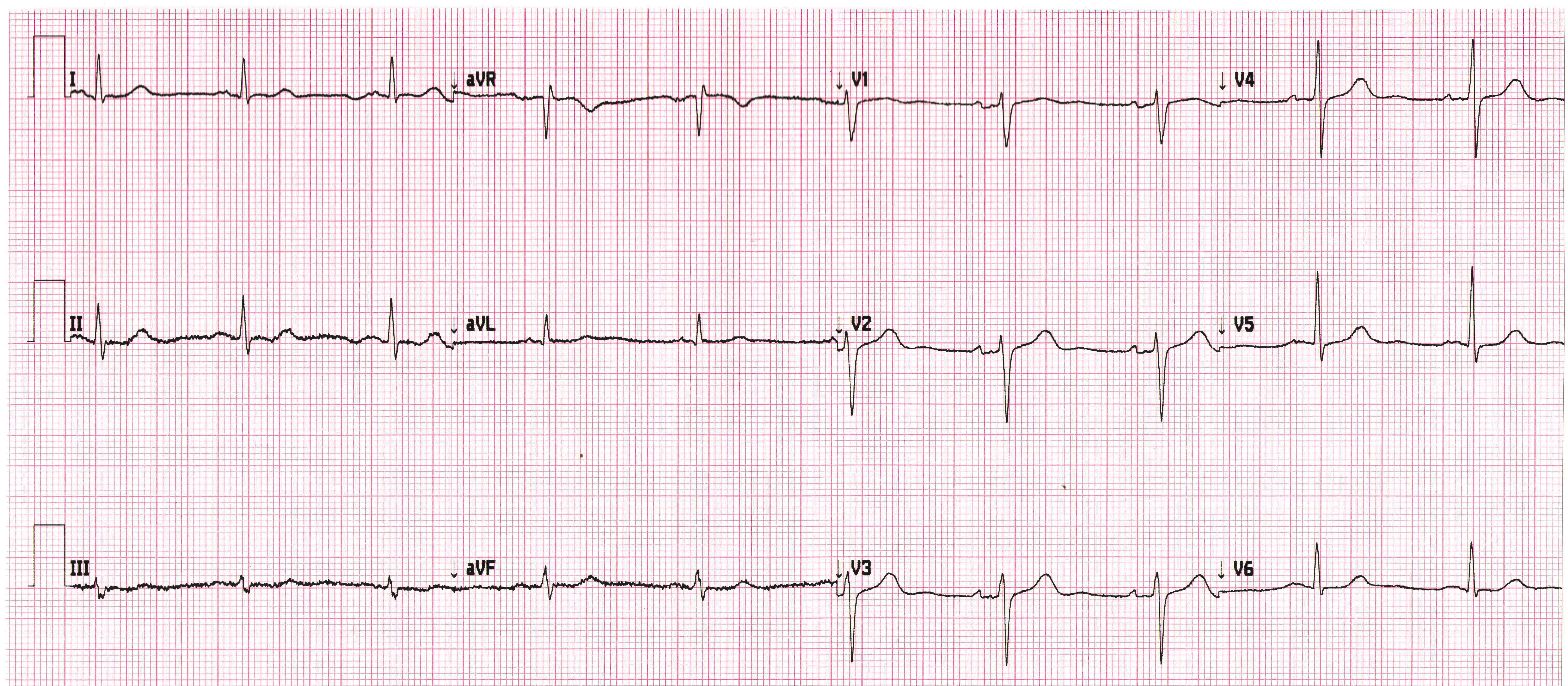
His blood pressure is 145/85mmHg. You arrange for an electrocardiogram and discuss the current situation.
1.What does the ECG show?
2.Why did Pharmac fund only two ACE inhibitors in 2002?
3. Which ACE inhibitors and angiotensin II receptor blockers (ARBs) are now funded in New Zealand?
4. Why is prescribing of cilazapril being discouraged by Pharmac and cilazapril/hydrochlorothiazide already discontinued?
5. What are the options for changing the combined cilazapril/ hydrochlorothiazide tablet to an alternative combined ACE inhibitor or ARB plus diuretic hypertension tablet?
a. If your patient had been taking only cilazapril 5mg daily, could he continue taking it?
6. What unique opportunity is currently present for treating hypertension?
a. What are the benefits of ARBs over ACE inhibitors for hypertension management?
7. What changes do you now make with your patient’s medication regimen?
a. What safety follow-up plans do you have for his blood pressure management?
b. What is the treated blood pressure target in 2021?
1. The ECG shows sinus rhythm, a normal axis and a rate of 60 beats per minute. It is normal, as for most patients with hypertension.
2. After its creation in 1993, Pharmac expanded a system known as “reference-based pricing” or “class effect”. Drugs that are judged, by Pharmac, to produce the same or similar therapeutic effect in treating the same or similar condition(s) are grouped together, and a single reimbursement level of reference pricing is set. Drugs above the reference price require part or total payment by the patient. In 2002, the rarely used ACE inhibitor drugs quinapril and cilazapril were funded.
3. Currently, cilazapril, quinapril, lisinopril, perindopril and enalapril are Pharmac funded ACE inhibitors for adult patients with hypertension. Losartan and candesartan are funded ARBs.
4. Most countries use ACE inhibitors other than cilazapril. In New Zealand, slightly more than half of the 500,000 annual ACE inhibitor prescriptions are for cilazapril. However, as most other countries do not use cilazapril, there is now only one manufacturer left that still makes it. Further, the combined cilazapril 5mg/hydrochlorothiazide 12.5mg tablet is no longer being manufactured.
5. The option is to simply swap cilazapril/hydrochlorothiazide to a combined diuretic with an ACE inhibitor or ARB. At approximately the equivalent strength, the funded tablets are quinapril 20mg/hydrochlorothiazide 12.5mg or losartan 50mg/hydrochlorothiazide 12.5mg. However, your patient’s blood pressure is a little high for a direct swap.
a. Yes, but as of 1 May, the prescription needs to note that this medication was being taken by the patient prior to 1 May. No new patients will be funded for cilazapril alone.
6. It is perfectly reasonable to simply change a patient from cilazapril to another funded ACE inhibitor. However, the limited supply of cilazapril, and the end of the supply of cilazapril/ hydrochlorothiazide, could be an opportunity to move to the equally efficacious but better tolerated ARB medications for hypertension.
a. A 2018 comprehensive review of ACE inhibitors and ARBs used in hypertension management, published in the Journal of the American College of Cardiology, concluded that ARB medicines are a better, safer option than ACE inhibitor medicines. The review states: “Given the equal outcome efficacy but fewer adverse events with ARBs, risk-to-benefit analysis in aggregate indicates that at present there is little, if any, reason to use ACE inhibitors for the treatment of hypertension.”
7. You elect to change the combined cilazapril 5mg/hydrochlorothiazide 12.5mg tablet to candesartan 16mg for two weeks, then 32mg long term. You ask your patient to return at two and six weeks to have his blood pressure reassessed. If his blood pressure remains high, you will add either chlorthalidone 12.5mg daily or indapamide 2.5mg each morning. This will be a stronger combination. Hence, he would then be taking four tablets each morning.
a. You plan to check creatinine and electrolyte levels at your two-week blood pressure review, and also two weeks after adding the diuretic, then every three to six months in the first year. You then plan to check them on an annual basis. You are aware that some patients have a significant fall in the serum sodium level or significant renal impairment with ACE inhibitors, ARBs or diuretic medicines.
b. You appreciate that your patient’s amlodipine dose could also be up-titrated in the medium term, as required for blood pressure control. For optimal blood pressure management, you are aiming for an average blood pressure of 130/80mmHg or below.
Chris Ellis is a consultant cardiologist at Auckland City Hospital, and at The Heart Group and Mercy Hospital, Auckland
Details of this case study have been changed to protect patient confidentiality
You can use the Capture button below to record your time spent reading and your answers to the following learning reflection questions:
- Why did you choose this activity (how does it relate to your PDP learning goals)?
- What did you learn?
- How will you implement the new learning into your daily practice?
- Does this learning lead to any further activities that you could undertake (audit activities, peer discussions, etc)?
Messerli FH, Bangalore S, Bavishi C, et al. Angiotensinconverting enzyme inhibitors in hypertension: To use or not to use? J Am Coll Cardiol 2018;71(13):1474–82.





![New Zealand Doctor Rata Aotearoa editor Barbara Fountain, RNZCGP president elect and Tauranga-based specialist GP Luke Bradford, Ministry of Health clinical chief advisor rural health Helen MacGregor, and Health New Zealand Te Whatu Ora clinical director primary and community care Sarah Clarke [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/1.%20Barbara%20Fountain%2C%20Luke%20Bradford%2C%20Helen%20MacGregor%20and%20Sarah%20Clarke.jpg?itok=091NETXI)
![Ngāti Porou Oranga specialist GP Elina Pekansaari and Te Nikau Hospital specialist in general practice and rural hospital medicine David Short [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/2.%20Elina%20Pekansaari%20and%20David%20Short.jpg?itok=h5XfSBVM)
![Locum specialist GP Margriet Dijkstra and OmniHealth regional operations manager (southern) Patricia Morais-Ross [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/3.%20Margriet%20Dijkstra%20and%20Patricia%20Morais-Ross.jpg?itok=jkrtRfJC)
![Golden Bay dairy farmer and dairy industry health and safety doctoral student Deborah Rhodes, and Golden Bay Community Health specialist GP Rachael Cowie [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/4.%20Deborah%20Rhodes%20and%20Rachael%20Cowie.jpg?itok=oM0_GcJc)
![Hauora Taiwhenua clinical director rural health Jeremy Webber, Australian College of Rural and Remote Medicine president Rod Martin and Observa Care director of business operations Deborah Martin, the wife of Dr Martin [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/5.%20Jeremy%20Webber%2C%20Rod%20Martin%20and%20Deborah%20Martin%2C%20the%20wife%20of%20Dr%20Martin.jpg?itok=P_aGmX_H)
![Spark Health chief executive John Macaskill-Smith and client director Bryan Bunz [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/6.%20John%20Macaskill-Smith%20and%20Bryan%20Bunz.jpg?itok=5yJvVZ0I)
![Associate dean (rural) Kyle Eggleton, third-year medical student Roselle Winter, and second-year pharmacy student Alina Khanal, all from the University of Auckland [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/7.%20Kyle%20Eggleton%2C%20Roselle%20Winter%20and%20Alina%20Khanal.jpg?itok=RQLd3TEs)
![Health New Zealand Te Whatu Ora clinical editor and specialist in general practice and rural hospital medicine Anu Shinnamon, and Whakarongorau chief clinical officer Ruth Large [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/8.%20Anu%20Shinnamon%20and%20Ruth%20Large.jpg?itok=i5TMswY9)
![Te Kahu Hauora Practice specialist GP Jane Laver and Ngāti Kahungunu ki Tāmaki-nui-a-Rua chief operations manager Tania Chamberlain [Image: NZD]](/sites/default/files/styles/thumbnail_cropped_100/public/2025-05/9.%20Jane%20Laver%20and%20Tania%20Chamberlain.jpg?itok=jtMklaCZ)