For older people and frail people, the long-term benefit of medicines reduces and the potential for harm from adverse effects increases. When the benefit–risk balance changes in this way, medicine review and optimisation are important to simplify the therapeutic regimen, reduce inappropriate medicines and minimise risks. In this article, pharmacist prescriber Linda Bryant uses two case studies to illustrate important considerations during medicine reviews
Don’t forget iron deficiency and thyroid function with gastric acid suppression
Don’t forget iron deficiency and thyroid function with gastric acid suppression

We are on our summer break and the editorial office is closed until 17 January. In the meantime, please enjoy our Summer Hiatus series, an eclectic mix from our news and clinical archives and articles from The Conversation throughout the year. This article was first published in the 31 March edition
The absorption of medicines for iron deficiency anaemia and hypothyroidism is affected by long-term proton-pump inhibitor use. This case study describes these interactions and the effect the prescribing cascade can have on thyroid function
This article has been endorsed by the RNZCGP and has been approved for up to 0.25 CME credits for the General Practice Educational Programme and continuing professional development purposes (1 credit per learning hour). To claim your credits, log in to your RNZCGP dashboard to record this activity in the CME component of your CPD programme.
Nurses may also find that reading this article and reflecting on their learning can count as a professional development activity with the Nursing Council of New Zealand (up to 0.25 PD hours).
- A sometimes neglected adverse effect of proton-pump inhibitors is iron deficiency anaemia.
- As with oral iron replacement preparations, the absorption of levothyroxine is also reduced, variably, by gastric acid suppression.
- Iron supplements themselves can also decrease levothyroxine absorption.
- Tapering to stop any unnecessary PPI use, and rescheduling doses of the PPI, oral iron and levothyroxine, can help reduce the adverse interactions of these medicines.
In 2003, Pharmac launched a campaign promoting appropriate and, for the majority, short-term use of proton-pump inhibitors. Likewise, BPACnz and the Goodfellow Unit have done similarly.
Proton-pump inhibitors (PPIs) remain an important long-term treatment for Barrett oesophagus and Zollinger–Ellison syndrome, and provide potential gastroprotection for patients using aspirin or an NSAID. However, the fact that PPIs remain in the top three most-prescribed medicines in Aotearoa New Zealand is challenging to justify as being appropriate. Studies (usually retrospective and observational) have presented evidence of an association between PPI use and many harmful sequelae, including infections, particularly Clostridium difficile and pneumonia.
One well-documented and sometimes neglected adverse effect is that of iron deficiency anaemia. Additional to this is a less well-documented interaction with levothyroxine.
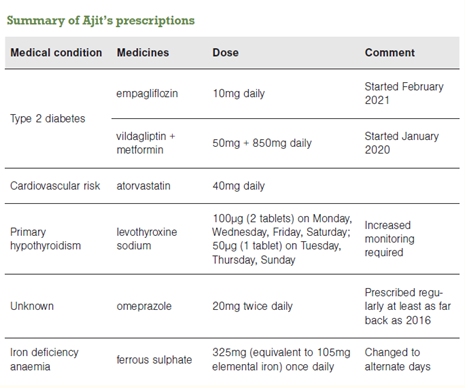
Ajit is a 73-year-old Indian man who has iron deficiency anaemia. He has been taking the PPI omeprazole 20mg twice daily for over five years without a clear rationale. His other medical conditions and treatments are presented in the table.
Ajit has complained of fatigue but no other symptoms. All investigations, including upper and lower endoscopies and coeliac antibody testing, have shed no light on the cause.
The mechanism of action of PPIs is through inhibition of the parietal cell hydrogen potassium ATPase (proton pump) with a resultant increase in gastric pH and hypochlorhydria or achlorhydria. Non-haem iron, found in vegetables, cereals, beans and lentils, requires an acidic pH for gastrointestinal absorption.1 For haem iron, this is not the case.
Vegetarians are, therefore, potentially more susceptible to iron deficiency in the context of hypochlorhydria or achlorhydria. Ajit confirms he has been a vegetarian all his life and is very careful to ensure all nutrients are included in his diet.
A less appreciated and less consistent potential adverse effect of PPI administration is levothyroxine malabsorption. In a manner not dissimilar to that described for iron, levothyroxine also requires an acidic environment for absorption.2 A recent systematic review has shown coadministration of levothyroxine and PPIs leads to a significant increase in thyroid-stimulating hormone (TSH) level.3 The levothyroxine formulation appears to be important and may account for variability in study outcomes.4
Ajit’s most recent thyroid function tests show his free T4 level in the upper-normal range at 20.9pmol/L, and his TSH level slightly above the normal range at 4.7mIU/L (reference range: 0.3–4.5mIU/L, which may differ between laboratories). These results are from tests performed during his current dosing regimen. Sequential readings were performed in 2020, all showing a TSH level just above the normal range.
Commonly, hypothyroidism is caused by Hashimoto disease, and this is usually progressive. It is not surprising, over months or years, to need to increase the amount of thyroxine replacement as further thyroid destruction occurs.
To add another layer to this scenario, iron replacement preparations can also increase TSH levels by decreasing levothyroxine absorption.5
It is confirmed that Ajit is not taking an over-the-counter NSAID or aspirin and does not have a health condition to warrant ongoing PPI use.
Recognising that abrupt cessation of a PPI can cause rebound hypersecretion of gastric acid, leading some people to believe they still need a PPI, this is discussed with Ajit. He opts to trial a decrease in omeprazole dose to 10mg twice daily as he is used to taking this medicine twice daily.
It is essential that the aim is PPI cessation, so allowing Ajit this level of control can be helpful. For instance, if he becomes symptomatic, he could use omeprazole 30mg daily for a short time. It is raised with him that going to once-daily dosing will be the next step. After that, it could be alternate days or on an as-required basis.
Ajit has medical insurance and is not concerned about medication costs. Therefore, a potential consideration is parenteral iron replacement using ferric carboxymaltose or iron polymaltose, but Ajit does not like the idea of an infusion and chooses to remain on oral iron.
A 2019 Goodfellow Gem (https://bit.ly/2OK0Gwy) gives confidence to advocate for alternate-day dosing of ferrous sulphate with potentially fewer adverse effects and a likely lower impact on levothyroxine.
Generally, the advice is for levothyroxine to be taken on an empty stomach with a glass of water in the morning, at least half an hour before food. For Ajit, this is more problematic – with his twice-daily dosing of omeprazole (optimal dosing), the PPI is also given first thing in the morning before breakfast.
This problem is discussed with Ajit. As an interim measure, he agrees to take the levothyroxine an hour before lunch and, while not perfect, to trial taking the iron supplement at night on alternate nights, recognising he will soon be dropping the night-time dose of his omeprazole. Ajit has no phone to record or remind him of his medicines administration, so he uses a small notebook to do this.
Given the omeprazole and iron dosing will be altered, Ajit’s thyroid function should be monitored monthly while the PPI is ceased, and hopefully the iron after that. If any thyroid dysfunction symptoms do appear, he should return to see you earlier.
Leanne Te Karu is a pharmacist prescriber working in primary care; Professor Bruce Arroll is a GP and head of department of general practice and primary health care at the University of Auckland
You can use the Capture button below to record your time spent reading and your answers to the following learning reflection questions:
- Why did you choose this activity (how does it relate to your PDP learning goals)?
- What did you learn?
- How will you implement the new learning into your daily practice?
- Does this learning lead to any further activities that you could undertake (audit activities, peer discussions, etc)?
We're publishing this article as a FREE READ so it is FREE to read and EASY to share more widely. Please support us and our journalism – subscribe here
- Schade SG, Cohen RJ, Conrad ME. Effect of hydrochloric acid on iron absorption. N Engl J Med 1968;279(13):672–74.
- Centanni, M. Thyroxine treatment: absorption, malabsorption, and novel therapeutic approaches. Endocrine 2013;43(1):8–9.
- Guzman-Prado Y, Vita R, Samson O. Concomitant use of levothyroxine and proton pump inhibitors in patients with primary hypothyroidism: a systematic review. J Gen Intern Med 2021; 19 January online.
- Virili C, Antonelli A, Santaguida MG, et al. Gastrointestinal malabsorption of thyroxine. Endocr Rev 2019;40(1):118–36.
- Irving SA, Vadiveloo T, Leese GP. Drugs that interact with levothyroxine: an observational study from the Thyroid Epidemiology, Audit and Research Study (TEARS). Clin Endocrinol 2015;82:136–41.